Dogs scratch, lick or chew because they are itchy; it is very unusual for a dog to do this simply out of habit.
A common cause of itchiness in dogs is allergy or atopy, a hereditary hypersensitivity to certain allergens. However, it is important to remember that not all itchiness is necessarily allergic. Bacterial or yeast infections, often secondary to hypersensitivity, can be highly itchy. This means the itch being experienced by a single itchy dog might have two or three causes: it might have an allergy, which has led in turn to a bacterial skin infection, and a yeast infection. Obviously in this case, all three causes must be addressed separately. There is no one medication that deals with all three causes of itching at once.
Other causes of itchiness apart from allergies might be parasites such as fleas, skin mites, and other blood sucking insects, fungal infections, immune mediated (abnormal activity of the body’s immune system) diseases and very occasionally some types of skin cancer.
In the days before the very efficient and safe flea treatments now available it was common to see fleas or other skin parasites causing problems. Now flea problems have become less important, although overreaction to flea bites does occur. Sarcoptic mite infestation, often called mange, is another parasitic disease that can mimic hypersensitivity, even when a very powerful diagnostic tool like a skin biopsy is used in the diagnostic process. Small numbers of mites can cause an extraordinary degree of itching.
Types of hypersensitivity reactions
Allergy is one of a class of responses by the body that are termed hypersensitivity reactions. These are harmful over-reactions by the body’s immune system. Hypersensitivity reactions can produce tissue injury and may cause serious disease.
They have been classified into four types. Allergy is a type I hypersensitivity, which means it is associated with IgE, a protein involved in allergen recognition. Allergic reactions occur when an individual animal which has already been sensitized to an innocent foreign substance (allergen or antigen) meets that foreign substance again and ‘over reacts’, usually within minutes.
Atopy or environmental hypersensitivity has been defined as the inherited predisposition to ‘over react’ to environmental allergens and develop antibodies (proteins that recognise other proteins from outside the body) against everyday substances that are inhaled, ingested or absorbed through the skin. The antibodies coat the surface of some cells and, by interacting with the ‘foreign invaders’, cause the coated cells to rupture, releasing their inflammatory contents into the skin. This promotes those clinical signs that are the hallmarks of atopy: itching, redness, and heat.
Many owners remark their animal’s skin feels hot to the touch when they are itchy. This is just another symptom of the dog’s allergy.
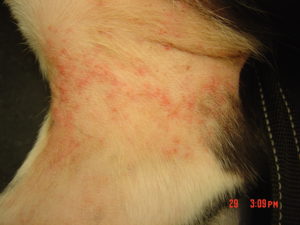
Red spots like this on flexor areas could be due to atopy
Given that the itchiness of one disease looks very much like the itchiness of another disease, how do we tell the diseases apart? The short answer is, with difficulty. There is no one test that can make the diagnosis of atopy. The veterinarian must make use of the individual dog’s history and that animal’s particular distribution of symptoms to draw up a list of the possible causes and then do tests to confirm or reject each diagnosis.
For a classic presentation of atopy to be present I would expect the ears, feet and face to be affected. In addition the flexor regions – the axillae (armpits), inguinal (groin) and lower leg areas – are often affected. The back or dorsum is usually spared.
In the majority of cases the onset of symptoms occurs between the ages of one to three years.
Genetic susceptibility
That there is a genetic or inherited component to atopy is shown by the fact that certain breeds and certain families within breeds are much more likely to get allergies than others. In my practice, the main breeds to suffer from environmental allergies are retrievers and terriers.
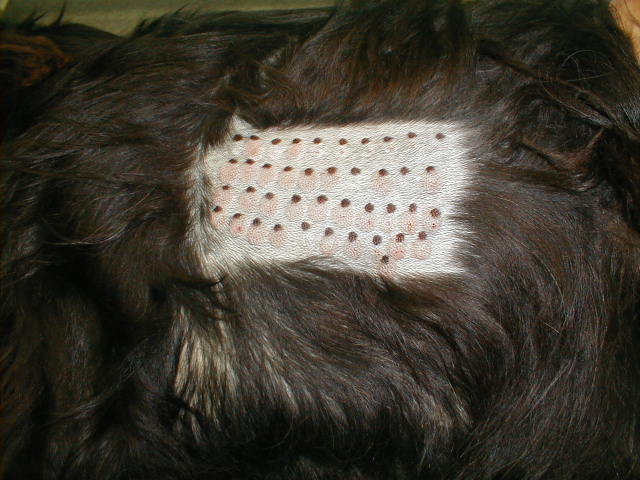
Intradermal skin test showing reaction to a number of allergens
Diseases that should be discounted before making the diagnosis of atopy or environmental hypersensitivity include adverse food reactions affecting the skin(cutaneous), ectoparasites, and contact hypersensitivity. To support the diagnosis of atopy, an intradermal test, similar to the scratch test in humans, can be done. A small amount of a specific antigen is injected into skin layers and the reaction compared with the reaction the skin makes to injected saline (negative control) or histamine (positive control). This tests allergen specific IgE in the skin and is considered the gold standard of testing for atopy. It is also possible to test for allergen specific IgE in the blood. This test can be used when the intradermal test isn’t available.
Allergy villain: the dust mite
In New Zealand, as in Europe, the most common allergen causing symptoms of allergy in dogs is protein in the excretions of the dust mite. There are two main species of this mite that commonly cause allergic reactions. They are Dermatophagoides farinae and D. pteronyssinus. Despite their common name they have little to do with dust. Both are free living mites that feed on shed skin.
The dust mite lives even in the cleanest bedroom – deep in carpets and curtains and in the seams of mattresses, where even the most house-proud individual can’t get rid of it. It thrives in poorly ventilated and humid homes. The excretion from the mites dries out and can be launched into the air when someone, including a dog, walks over a rug, sits on a chair, or jumps on the bed, giving allergic people and animals immediate symptoms. Unlike pollen, dust mites are present all year round causing constant allergy. Pollens of many trees, weeds and grasses can also give rise to the symptoms of canine atopy. This is usually seasonal.
Treatment
The treatment of canine atopy is a multi-pronged attack: lower the exposure if possible, improve the skin barrier, treat the symptoms and consider allergen specific immunotherapy (anti-allergy shots). Avoidance is often impossible, particularly in the case of inside-dwelling dogs with a dust mite allergy, though a reduction in exposure can often be achieved through careful management. The skin barrier can be improved with topical products like Essential 6 which increase the protective oils in the skin. Several commercial diets do so too. Treatment of the symptoms of severe itch and inflammation can be achieved with the potent anti-itch drug Apoquel, or with corticosteroids. Soothing shampoos and washes are helpful. Often secondary skin infections need to be treated with antibiotics or topical washes. Immunotherapy is not universally successful but it does offer the one alternative to a lifetime of medication if avoidance is impossible.
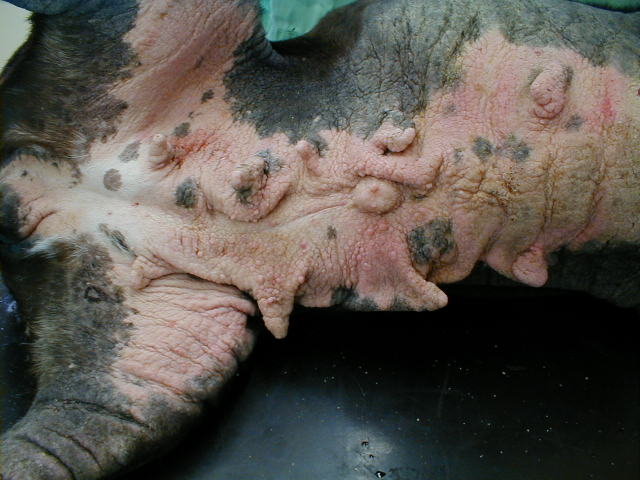
End-stage skin disease in a dog with chronic atopy with secondary yeast infections
Duncan Graham BSC(Hons) BVSc. Duncan is a former partner at Halifax whose practice Animal Dermatology is exclusively focussed on skin diseases of pets. He covers all of the South Island and the lower North Island. He is normally found at Halifax Vet Centre on alternate Thursday mornings.

Recent Comments